Breathing changes can be easy to dismiss at first. Some patients notice mild shortness of breath, occasional chest tightness, or reduced stamina and assume it is stress, aging, or deconditioning. In primary care, those symptoms deserve a closer look because they may reflect early changes in lung function even before a patient understands what is causing them. BluePoint Medical Group presents pulmonary evaluation as part of a broader diagnostic and preventive care model, which aligns well with patients who want clarity without unnecessary alarm.
That is where pulmonary testing helps evaluate breathing concerns in a more objective way. These studies, often called pulmonary function tests or lung function tests, measure how well the lungs move air, how much air they hold, and how effectively gases pass from the lungs into the blood. This information gives a healthcare provider more than a symptom description alone and can support earlier, more accurate next steps.
Patients often come in wanting to know whether their breathing problem is serious, temporary, or related to a chronic condition already on their chart. A careful function test does not answer every question by itself, but it helps transform vague symptoms into measurable findings. That can make the conversation more focused and less uncertain for both the patient and the clinician.
Intermittent Shortness of Breath Still Deserves Attention
Intermittent symptoms are still worth discussing, especially when they begin to affect exercise, sleep, work, or daily routines. Not every episode of breathlessness signals lung disease, but repeated symptoms may point to airway narrowing, reduced reserve, inflammation, or a cardiopulmonary issue that needs follow-up. Many respiratory problems begin gradually, so it is common for patients to normalize them before seeking care.
This is one reason early detection matters. A patient may not have severe symptoms yet, but testing may still identify abnormal lung function, reduced airflow, or signs that the lungs are not exchanging gases as efficiently as expected. Finding those patterns earlier may shape monitoring, medication review, or referral decisions before symptoms become more disruptive.
Risk also depends on context. Smoking history, dust exposure, respiratory infections, allergy patterns, asthma history, occupational irritants, and other risk factors all influence how a provider interprets breathing concerns. A mild symptom in one patient may deserve a different level of attention in another depending on their history and exam.
Pulmonary Function Tests and What They Measure
Pulmonary function tests PFTs are a group of studies designed to assess how well the respiratory system is working. They may evaluate airflow, lung volume, and gas exchange, which together provide a broader picture of how the lungs work than symptoms alone ever could. Medline Plus and the American Lung Association both describe these tests as a way to check lung performance and help diagnose or monitor lung problems.
Some tests focus on how much air a person can inhale or exhale. Others look at whether the lungs can transfer oxygen-related gases efficiently into the bloodstream. In practice, that means pulmonary function testing helps answer several patient-centered questions at once: Are the airways narrowed, are the lungs restricted, and are the lungs moving gases across the air sacs the way they should?
These studies are especially helpful because many breathing complaints overlap. Asthma, deconditioning, chronic bronchitis, restrictive scarring, and even non-lung issues can all feel similar from the patient’s perspective. Objective testing allows the provider to decide whether the findings point toward obstructive lung diseases, restrictive lung diseases, or the need for other tests.
Spirometry as a Core Test for Checking Lung Function
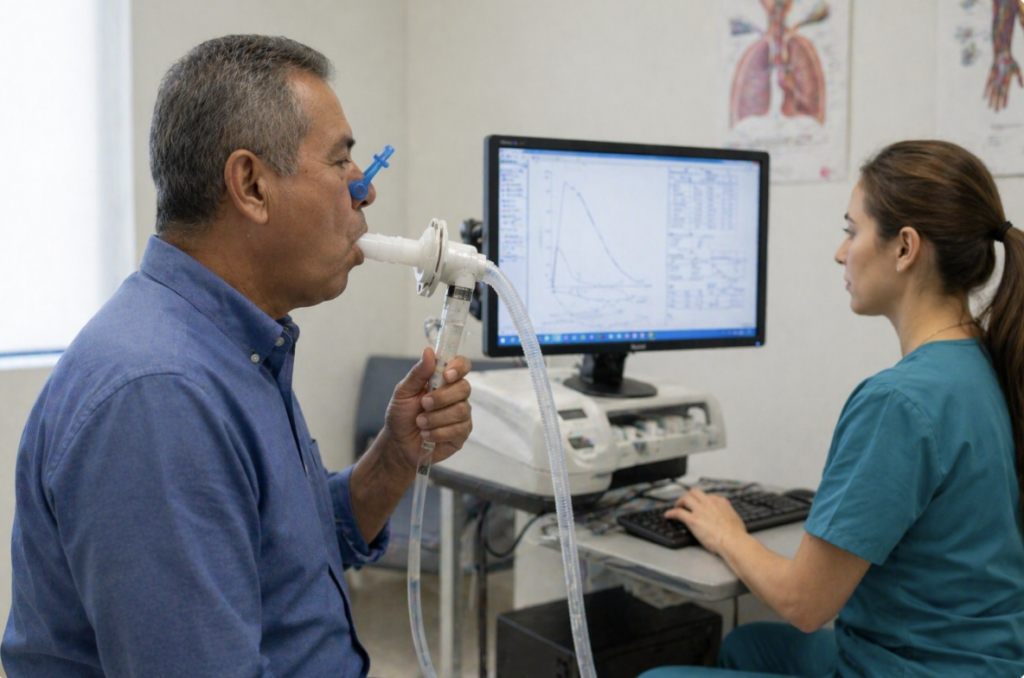
The most common breathing study is the spirometry test. During pulmonary function tests, spirometry, a patient takes a deep breath and blows out as forcefully and completely as possible through a mouthpiece connected to a measuring device. This test is central because spirometry measures both the amount of air exhaled and how quickly that air comes out.
Important spirometry values include forced vital capacity, forced expiratory volume, and the ratio between them. In simpler terms, the test helps show whether the lungs can empty normally and whether airflow is being limited. These measures are often compared with predicted normal values based on age, height, sex, and other reference standards.
This matters because spirometry may detect narrowing in the bronchial tubes and may help a healthcare provider diagnose or monitor conditions such as asthma and chronic obstructive pulmonary disease. It is often one of the first tests used when patients report cough, wheeze, exertional symptoms, or ongoing breathlessness.
Forced Vital Capacity and Forced Expiratory Volume Explained
Patients often see technical terms on reports and are not sure what they reflect. Forced vital capacity refers to how much air a person can blow out after taking the deepest breath possible. Forced expiratory volume usually refers to how much of that air comes out in the first second, which helps clinicians judge airflow limitation.
When these measures fall outside the expected range, the pattern can suggest either obstruction or restriction. That distinction is clinically useful because the treatment approach and follow-up questions may be very different. The purpose is not just to label the result, but to connect the result to the patient’s symptoms and possible diagnosis.
Results still require interpretation. A low number does not automatically define a disease on its own, and a value near the lower end of normal may matter more in one patient than another. That is why pulmonary function test results are most meaningful when reviewed alongside history, medications, exposures, and physical findings.
Why Lung Volume Testing Adds More Detail
A lung volume test goes beyond simple airflow and examines how much air the lungs can hold overall. This can be measured through methods such as body plethysmography, which helps estimate total lung capacity and how much air remains after exhalation. The American Thoracic Society explains that this adds important information about trapped air and overall breathing mechanics.
This is particularly helpful when a provider suspects a restrictive pattern or wants to better understand why a patient feels limited. If lungs cannot fully expand, or if too much air remains trapped after exhaling, symptoms may feel similar even though the underlying mechanism is different. That is one reason lung volumes are often paired with spirometry rather than used alone.
For patients, this added detail may support a more accurate workup for pulmonary fibrosis, chest wall restriction, severe obstruction, or other lung conditions affecting mechanical breathing performance. It also helps clarify whether symptoms reflect reduced capacity, air trapping, or a mixed pattern that needs broader interpretation.

Lung Diffusion Capacity Testing and Gas Exchange Evaluation
A lung diffusion capacity test, also called a diffusion capacity test, measures how well gases move from the lungs into the blood. In many labs, the measured gas involves a very small amount of carbon monoxide, because it helps estimate how effectively gases cross the lung membrane. This is different from airflow testing and focuses more on whether the lungs absorb oxygen efficiently.
Patients sometimes ask why a test would involve carbon monoxide at all. The reason is technical: the measurement estimates how much carbon monoxide passes across the lungs under controlled conditions, which helps clinicians infer how well the lungs handle gas exchange. It is not the same as exposure to harmful environmental carbon monoxide.
This type of result may be useful in suspected interstitial lung disease, emphysema, pulmonary vascular issues, or unexplained exertional symptoms. If diffusion is reduced, a provider may look more closely at why the lungs are not transferring gases as expected and whether further cardiopulmonary evaluation is needed.
Can pulmonary testing help diagnose asthma, COPD, or pulmonary fibrosis?
Yes, these tests are commonly used as part of the evaluation for several respiratory disorders. Spirometry may help diagnose asthma, monitor chronic obstructive pulmonary disease, and assess conditions such as chronic bronchitis that affect airflow. Tests may also support evaluation of restrictive patterns seen in pulmonary fibrosis and other scarring conditions.
That said, testing is one part of diagnosis rather than the whole diagnosis. A clinician still considers symptoms, smoking history, triggers, imaging, oxygenation, and exam findings before making conclusions. Pulmonary testing supports the reasoning process by showing whether the breathing pattern fits what the patient is experiencing.
The same cautious approach applies to other disorders, such as cystic fibrosis or chronic inflammatory airway disease. A result may suggest that something deserves more attention, but diagnosis and management depend on the full clinical picture rather than a single number.
When Exercise Tests or Six-Minute Walk Testing Are Used
Not every respiratory evaluation ends with office spirometry. Some patients may need exercise tests, a six-minute walk test, or even cardiopulmonary exercise testing when symptoms occur mainly with exertion. These approaches can add information about endurance, oxygen response, and cardiopulmonary performance during activity.
These studies may be useful when the question is less about baseline airflow and more about functional limitation. For example, they may help evaluate unexplained shortness of breath, monitor disease progression, or track response to treatment over time. They are often considered when resting measurements do not fully explain what the patient feels during daily activity.
From a patient perspective, this matters because breathing symptoms are not always captured by one office measurement. Sometimes the most useful information comes from seeing what happens during walking or structured exertion, especially when symptoms only appear with physical effort.
What Pulmonary Test Results Do and Do Not Tell You
The biggest benefit of pulmonary testing is clarity. These breathing tests may reveal abnormal lung function, show whether airflow is obstructed, estimate lung volume, and help explain why symptoms are happening. That information can support personalized treatment plans, medication review, and better monitoring of respiratory health over time.
There are also limits patients should understand. A test may be influenced by effort, technique, recent respiratory illness, or whether the patient used breathing medicines before the study. Some values may fall outside the normal range temporarily, and some patients need repeat testing before a pattern is clear.
Testing also does not replace other parts of care. A provider may still consider pulse oximetry, imaging, cardiac review, or broader medical procedures depending on symptoms, blood pressure, and exam findings. In other words, pulmonary testing is powerful because it adds objective data, not because it answers every question by itself.

FAQ
What are pulmonary function tests used for?
They are used to check how well your lungs move air, hold air, and transfer gases. Providers use them to help evaluate symptoms, monitor lung conditions, and support diagnosis alongside other clinical findings.
Does spirometry hurt?
Spirometry is usually not painful, but it can feel tiring because you have to inhale deeply and blow out hard. Some patients feel briefly lightheaded after the breathing effort.
Can pulmonary testing diagnose asthma or COPD?
It can be an important part of diagnosis, especially spirometry, but it is not the only factor. Your provider also considers your symptoms, history, exam, and sometimes additional testing.
Why would I need more than one lung test?
Different tests answer different questions. Spirometry looks at airflow, lung volumes assess how much air your lungs hold, and diffusion testing evaluates how well gases move from the lungs into the blood.
Conclusion
When breathing changes persist, objective testing can make the next step more informed. Pulmonary function tests offer measurable insight into airflow, vital capacity, gas transfer, and how well your lungs are performing under current conditions. That information may support early detection, guide a treatment plan, and help determine whether symptoms reflect a temporary issue or a more established respiratory condition.
BluePoint Medical Group positions pulmonary evaluation within a broader primary care setting focused on prevention, diagnosis, and long-term follow-up. That kind of continuity matters because breathing concerns are often easier to understand when test findings are reviewed together with your symptoms, history, medications, and risk profile.
If you have ongoing airway symptoms, reduced exercise tolerance, or breathing changes that do not feel normal, schedule a consultation with BluePoint Medical Group to discuss whether pulmonary testing is appropriate and what your results may mean for your next step in care.