When patients hear that a test has been ordered, they often think of illness first. In primary care, though, diagnostic testing is usually part of a broader effort to understand symptoms, track risk factors, and build a clearer view of overall health before problems become harder to manage. That is one reason diagnostic testing helps doctors see the full health picture rather than relying on symptoms alone.
At BluePoint Medical Group, this fits the practice’s focus on primary care, preventive medicine, chronic condition management, and on-site diagnostic support. Bloodwork, EKGs, and related testing are presented as tools that support timely, informed care instead of one-time snapshots disconnected from the rest of a patient’s medical history.
That distinction matters because the full health picture is rarely found in one conversation or one symptom. It often comes from combining medical history, physical findings, screening tests, blood analysis, and imaging test results so the healthcare provider can understand what is changing, what may need additional testing, and what may simply need monitoring over time.
Symptoms Alone Do Not Always Explain Health Issues
Many health issues develop gradually. A patient may notice fatigue, chest discomfort, digestive tract issues, or weight change, but symptoms alone do not always show whether the cause relates to inflammation, hormone shifts, high cholesterol, infection, medication effects, or another condition entirely. Diagnostic testing gives doctors more objective findings to interpret alongside what the patient is feeling.
Symptoms can also overlap across many conditions. Shortness of breath, for example, may relate to asthma, heart strain, anxiety, infection, or another illness. Without testing, there is a greater chance of unnecessary anxiety, delayed care, or treatment planning based on incomplete information.
That is why primary care often starts with both conversation and evidence. A doctor listens to the patient’s symptoms, reviews family history and risk profile, and then decides whether lab work, imaging, or screening is appropriate to detect early changes or rule out more serious disease.
Diagnostic Tests That Help Build a Fuller Picture of the Body
In primary care, diagnostic testing may include blood analysis, urine testing, EKGs, and different forms of diagnostic imaging depending on the concern. These tests look at different major systems of the body, which helps the healthcare team move from general suspicion to a more accurate clinical understanding.
Bloodwork often provides some of the earliest clues. Glucose, kidney function, liver markers, cholesterol levels, and C-reactive protein or related inflammatory markers may provide insights into cardiovascular risk, diabetes concerns, kidney stress, or ongoing inflammation that is not obvious from symptoms alone.
Imaging works differently by helping doctors create pictures of structures inside the body. Depending on the situation, this may involve X-ray, CT scan, MRI scans, or ultrasound imaging, each chosen for a different reason and level of detail.
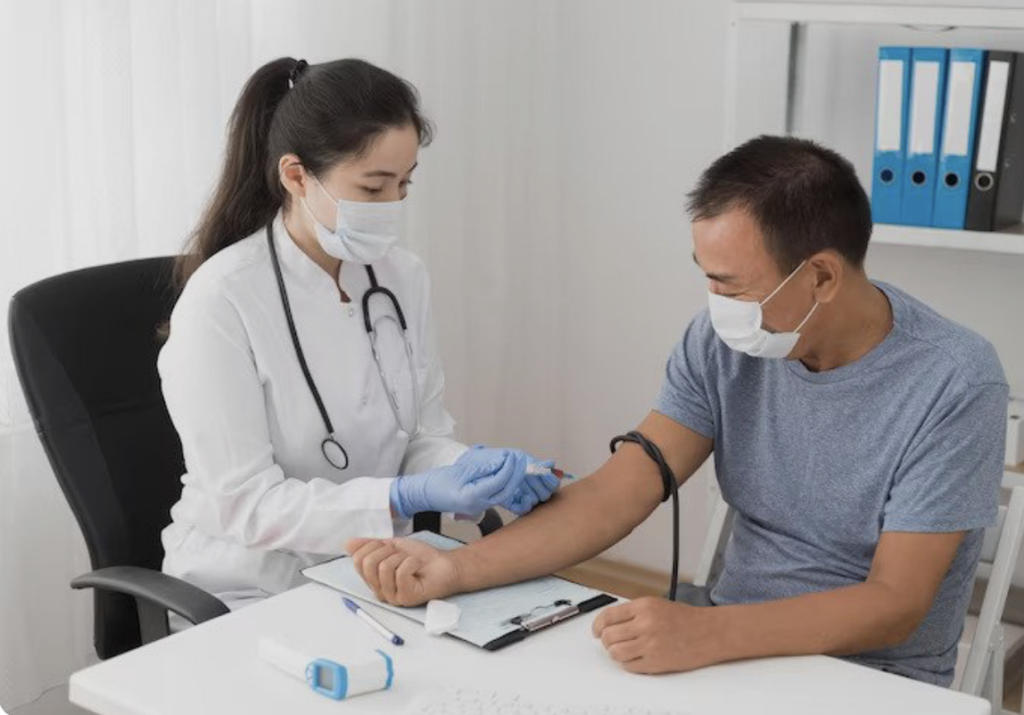
Blood Analysis in Early Detection and Treatment Planning
A routine lab panel may seem simple, but it can reveal early signs of disease before symptoms become severe. Blood sugar trends may point to diabetes risk, while cholesterol levels and inflammation markers may influence how a doctor evaluates heart disease risk and whether lifestyle changes or medication should be discussed.
Blood analysis also helps when symptoms are vague. Weakness, swelling, dizziness, or fatigue may relate to electrolyte shifts, anemia, kidney function, infection, thyroid changes, or medication effects. In these cases, testing adds clarity and may prevent treatment from being based on guesswork.
For long-term care, lab findings also matter because they provide a baseline. When results are repeated over time, the care team can compare changes, monitor chronic disease, and decide whether a patient needs continued observation or additional testing.
When Diagnostic Imaging Adds More Detail Than Lab Work Alone
Lab work may show that something is off, but imaging may show where the problem is and how it affects the body. Diagnostic imaging lets doctors look inside the body for clues about a medical condition, using different technologies to examine bones, organs, soft tissues, and blood vessels in greater detail.
An X-ray is often useful for bones and certain chest concerns because X-ray images can be obtained quickly, sometimes in just a few minutes. In simple terms, an X-ray tube sends a controlled beam through the body to create pictures based on how different tissues absorb that energy.
When more detail is needed, a CT scanner may be used. Computed tomography combines many X-ray views to create cross-sectional images, which may be useful for trauma, internal bleeding, kidney stones, lung findings, or selected signs of cardiovascular disease.
CT Scans, MRI Scans, and Radiation Exposure in Patient Care
A CT scan and an MRI are both valuable, but they are not interchangeable. CT uses X-rays and is often chosen when speed matters or when doctors need a detailed view of structures such as the lungs, bones, or possible bleeding. MRI uses magnets and radio waves and is especially useful for selected soft tissues, the brain, the spinal cord, and joint concerns.
Because CT uses ionizing radiation, radiation exposure is one factor doctors consider before ordering the test. NIH notes that CT remains an important diagnostic tool, but like any medical test, it should be used thoughtfully based on the clinical question rather than routinely without a reason.
Some CT or MRI studies may also use a contrast medium or contrast dye to make certain structures easier to see. Whether contrast is needed depends on the area being studied, kidney function, allergy history, and the specific findings the provider is trying to clarify.
Ultrasound Imaging for Blood Flow and Cardiovascular Risk Review
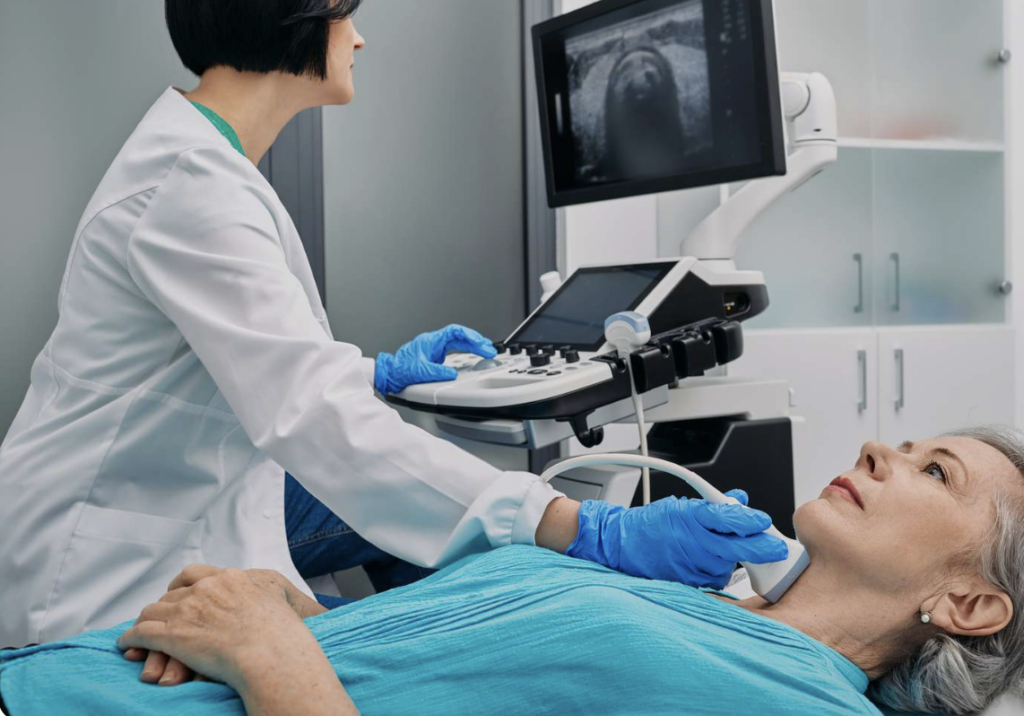
Ultrasound imaging uses sound waves rather than radiation, which makes it useful in many situations where doctors want a real-time view without X-ray exposure. It can assess organs, selected soft tissues, and, in vascular studies, it can also help visualize blood flow.
A carotid ultrasound is one example. MedlinePlus explains that carotid duplex testing shows how well blood is flowing through the carotid arteries, which supply blood to the brain. This may matter when evaluating stroke risk, plaque buildup, or a broader cardiovascular risk picture.
In primary care, tests like this are usually ordered based on symptoms, exam findings, and risk factors such as high blood pressure, smoking history, diabetes, or family history. These diagnostic tests are not for everyone, but when they are appropriate, they may provide valuable insights into blood vessels and circulation.
Screening Tests in Cancer and Preventive Care Decisions
Screening tests are different from diagnostic tests ordered for symptoms, but they also help doctors see the full health picture. Screening is used when a patient does not yet feel sick, with the goal of early detection for conditions such as breast cancer and lung cancer, where earlier identification may improve treatment options.
Cancer screening is not one-size-fits-all. Age, smoking exposure, symptoms, and family history all influence what is recommended and when. The benefits of diagnostic testing are strongest when a primary care provider reviews personal risk rather than ordering every available test.
The same caution applies to prostate cancer. Screening conversations should be individualized because benefits and tradeoffs vary by patient. In other words, more testing is not always better unless it matches the patient’s actual risk profile and values.
Family History in Diagnostic Decision-Making
Family history can shape how doctors interpret symptoms and which tests they consider first. A patient with relatives affected by coronary artery disease, diabetes, or certain cancers may have a different risk profile than someone without those patterns, even when their current symptoms are mild, which is one reason adults benefit from regular primary care visits.
This does not mean family history determines the future. It means it adds context. If a patient has a strong family history of heart disease along with blood pressure issues or high cholesterol, a provider may pay closer attention to cardiovascular disease prevention and follow-up.
That is one reason the best testing decisions usually happen inside an ongoing primary care relationship. When the healthcare provider knows the patient’s background, prior results, and concerns, testing can be more targeted and more useful.
Bone Density Testing and Body Scans Do Not Replace Regular Primary Care
Patients sometimes assume that a full body scan or a broad “body scans” package will answer every health question. In reality, routine primary care relies on targeted testing because tests are most helpful when they respond to symptoms, screening guidelines, exam findings, or known risk factors. Broad testing without context may increase cost and lead to findings that do not improve care.
Bone density testing is a better example of targeted prevention. A DEXA scan is a low-dose X-ray used to measure bone health and fracture risk, especially in patients whose age, history, or medications raise concern for weakening bones.
Used this way, testing supports proactive steps rather than confusion. It helps patients and providers focus on what is most relevant to long-term health instead of assuming every test is necessary for everybody.
Why the Right Test Matters More Than More Tests
The main benefit of diagnostic testing is clarity. A thoughtful combination of symptoms, medical history, screening, lab findings, and imaging can help detect early disease, confirm or rule out concerns, and guide treatment decisions with more confidence.
At the same time, good testing is selective. It weighs the benefits, timing, cost, patient preference, and possible downsides such as false positives, unnecessary anxiety, or avoidable radiation exposure. Thoughtful preventive testing balances these factors as part of evidence-based care, not as a sign that providers are being overly cautious.
When patients understand why a test is being ordered, what it may show, how to prepare, and whether a full report could lead to additional testing, they are in a better position to make informed decisions with their care team. Knowing what to expect from diagnostic testing supports that understanding, and that kind of transparency is central to patient-centered primary care.

FAQ
How do doctors decide which diagnostic test I actually need?
Doctors usually start with your symptoms, medical history, exam findings, and risk factors. From there, they choose the test most likely to answer a specific clinical question rather than ordering everything at once.
Is a CT scan better than an MRI?
Not always. A CT scan and an MRI serve different purposes, and the best option depends on what part of the body is being examined and what your provider needs to see in greater detail, as part of broader preventive and primary care testing.
Can screening tests find cancer before symptoms start?
Yes, some screening tests are designed for that purpose. CDC notes that regular screening may detect certain cancers early, including breast, cervical, colorectal, and lung cancers.
Conclusion
Diagnostic testing is most useful when it is connected to the patient’s real story. Blood analysis, screening, ultrasound imaging, X-ray, CT, and MRI each offer different forms of information, but none of them matter in isolation. Their value comes from how they fit with symptoms, family history, risk factors, and the goals of ongoing care.
That is why diagnostic testing helps doctors see the full health picture. It may detect early changes, sharpen cardiovascular or cancer risk assessment, clarify unexplained symptoms, and guide next steps with greater detail. It also helps reduce the chance that important findings will be missed simply because a condition was still developing quietly.
BluePoint Medical Group approaches testing as part of integrated primary care rather than as a stand-alone service, with convenient on-site bloodwork and specimen collection. Schedule a consultation with BluePoint Medical Group to review symptoms, screening needs, and diagnostic options in a setting designed around informed decisions and long-term health planning.