Routine monitoring helps doctors track changes in health because many conditions develop gradually rather than all at once. A patient may feel mostly fine while blood pressure, blood sugar, weight changes, or sleep disruption are already affecting daily functioning. When these changes are reviewed over time, healthcare providers can build a more accurate picture of overall health and treatment response.
For BluePoint Medical Group, this topic fits naturally within primary care, diagnostics, preventive medicine, and chronic disease management. The goal is not to create alarm. The goal is to give patients and healthcare professionals better access to useful health data so informed decisions can happen earlier and with more context.
Important Health Trends Patients May Miss Between Visits
Many patients only think about symptoms during an illness or a stressful week. That can make it harder to notice trends involving fatigue, medication use, body temperature, heart rate, or stress. A single appointment may capture one moment, but it may not show what has been happening across daily life.
This matters because many chronic diseases change slowly. Hypertension, diabetes, asthma, and some heart-related concerns often require repeated review rather than one isolated reading. Without routine monitoring, providers may have less detail for treatment planning and fewer opportunities for early detection.
What Routine Health Monitoring Actually Includes
Routine health monitoring may include office visits, home readings, lab work, symptom tracking, and selected devices that provide insights into day-to-day patterns. Depending on the patient, this can involve blood pressure logs, glucose readings, weight changes, sleep patterns, pulse checks, and updates about medication effects.
This kind of monitoring is not only for severe illness. It is often beneficial for preventive care, follow-up after a diagnosis, and ongoing management of many conditions. It gives doctors a more complete view of the body over time instead of relying only on occasional doctor observations.
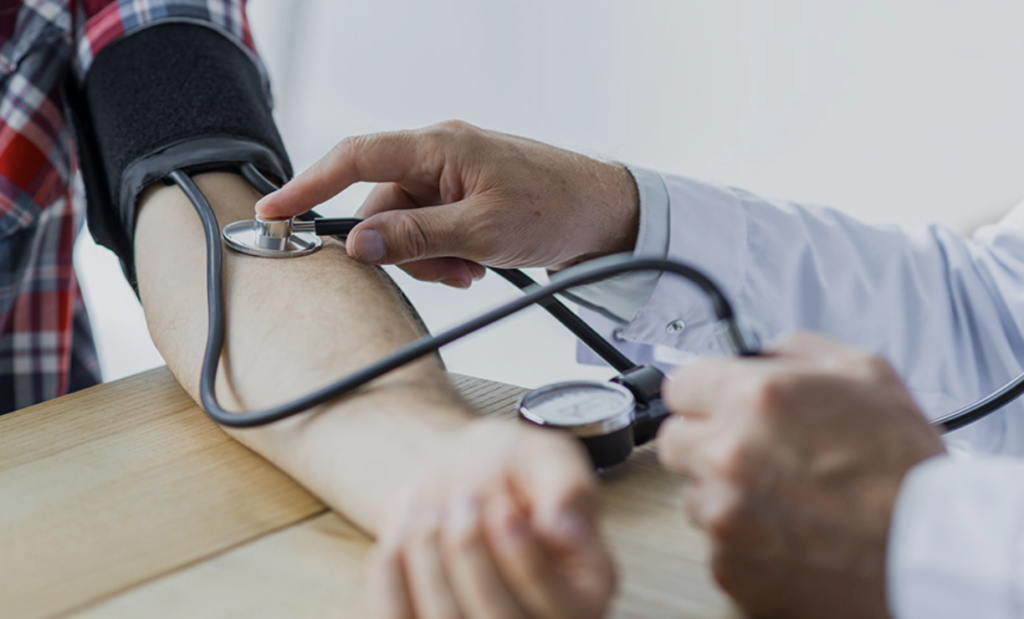
Routine Monitoring for Early Detection and Better Health Outcomes
One of the biggest benefits of regular monitoring is enabling early detection. When doctors identify trends sooner, they may be able to adjust medication, recommend testing, or address risk factors before symptoms become harder to manage.
That does not guarantee a specific result, but it may support better health and better health outcomes. Early detection is especially important when patients are at risk for heart disease, diabetes complications, or worsening hypertension. It also gives the healthcare team more time to respond thoughtfully instead of urgently.
The Importance of Blood Pressure Monitoring in Primary Care
Blood pressure is one of the clearest examples of why monitoring matters. Readings can vary across settings, and home tracking may help identify trends that are not obvious during a brief office visit. This is one reason self-measured blood pressure monitoring is widely used in hypertension care.
For many patients, blood pressure monitoring supports decisions about medication, lifestyle changes, and follow-up timing. It may also help providers evaluate how stress, exercise, or medication effects are influencing heart health over time. That makes it a practical tool, not just a number on a chart.
Continuous Glucose Monitors and Blood Sugar Tracking as Clinical Insights
For patients with diabetes, continuous glucose monitors can be a game-changer because they show how glucose levels change throughout the day and night. Instead of relying only on occasional fingerstick checks, patients and doctors can review patterns related to meals, sleep, activity, and medication.
This type of health data can be useful in monitoring chronic conditions and reducing guesswork. It may help the care team identify trends, discuss symptoms more clearly, and make more informed decisions about treatment planning. Not every patient needs a CGM, but for some, it adds meaningful detail to diabetes management.
The Role and Limits of Wearable Devices in Medical Care
Wearables and home devices may offer helpful insights, especially for heart rate, sleep, physical activity, and selected symptoms. Tools like an Apple Watch or pulse oximeters can support awareness and give patients more information to share with providers.
Still, these devices do not replace clinical judgment. Pulse oximeter readings can be affected by motion and other factors, and consumer tools are best used as part of a larger conversation with healthcare professionals rather than as a stand-alone diagnosis.

Remote Patient Monitoring in Chronic Disease Management
Remote patient monitoring allows parts of care to continue between in-person visits. This may include home blood pressure readings, glucose tracking, symptom updates, or digital communication that helps providers review changes more consistently.
For patients managing chronic conditions, this approach can support ongoing care without making every concern dependent on an office visit. In primary care, that may improve access, strengthen communication, and help doctors respond to findings sooner when trends suggest a patient needs closer review.
Why Doctors Need More Than Numbers Alone
Numbers matter, but they are not the whole story. Providers also need to understand the patient’s symptoms, sleep, stress, medication use, daily activities, and how the body is functioning in real life. A normal-looking value may still need context if the patient feels worse, has new limitations, or reports side effects.
That is why effective monitoring combines data with conversation. The most useful care plans are built when providers look at trends alongside the patient’s lived experience, goals, and barriers to change. This creates more personalized care and stronger long-term management.
What Patients Should Know Before Tracking More Health Data
Routine monitoring offers many benefits. It may help identify trends, support earlier action, clarify medication effects, and give the healthcare team a stronger basis for treatment decisions. For some patients, it also improves confidence because they better understand what is changing and why it matters.
At the same time, more data is not always better if it causes confusion or anxiety. Monitoring should fit the person, the condition, and the treatment plan. Results vary; some devices have limitations, and any concerning findings should be reviewed with a licensed medical provider rather than interpreted alone.

FAQ
How often should I monitor my blood pressure at home?
That depends on your diagnosis, medication, and provider’s guidance. Many patients with hypertension are asked to check it regularly for a period of time, so trends are easier to review.
Are continuous glucose monitors only for people with diabetes?
They are mainly used for people with diabetes, especially when glucose control needs closer review. Your provider can tell you whether this tool is appropriate for your treatment plan.
Can a smartwatch diagnose heart problems?
No, a smartwatch may provide useful data, but it does not replace a medical evaluation. Concerning symptoms or abnormal readings should always be discussed with a healthcare professional.
Is remote patient monitoring the same as telehealth?
Not exactly. Telehealth usually refers to virtual visits, while remote patient monitoring focuses on sharing health data from home so providers can review trends between appointments.
Conclusion
Routine monitoring helps doctors track changes in health more effectively because it turns scattered information into useful patterns. Whether the concern involves blood pressure, blood sugar, sleep, stress, medication, or chronic disease follow-up, regular monitoring can give providers a clearer understanding of what is happening over time.
For patients, that often means more personalized care, better conversations, and earlier opportunities to respond when health metrics begin to shift. It also supports preventive care by helping the healthcare team identify risk factors before they cause more disruption to quality of life.
BluePoint Medical Group integrates primary care, diagnostics, preventive care, and chronic disease management in a way that supports ongoing health monitoring and informed decisions. Schedule a consultation with BluePoint Medical Group to review symptoms, discuss monitoring tools, and build a care plan that reflects your health goals and daily reality.