Many patients do not ignore their health on purpose. More often, everyday life gets busy, symptoms seem minor, and a doctor’s office visit feels easy to postpone. Over time, though, the details that seem small at first can shape overall health, affect diagnosis, and influence how quickly a physician or other provider can move toward the best care. At BluePoint Medical Group, that day-to-day reality is why primary care remains such an important part of long-term wellness in Las Vegas.
When people search for what doctors wish patients paid more attention to, they are often looking for something practical rather than dramatic. They want to know what actually matters during appointments, what information should be shared, and which habits influence preventive care, blood pressure, chronic disease monitoring, and decisions about specific treatment. That perspective is especially valuable in family medicine and internal medicine, where the goal is not just treating one problem in one moment, but understanding the whole person across time.
BluePoint Medical Group presents primary care physicians, diagnostics, and ongoing wellness support as part of a connected care model focused on prevention, early evaluation, and continuity. That matters because many medical concerns are easier to understand when there is a record of prior visits, test results, medications, symptoms, and family risk. For patients alike who want a more organized, informed approach to health care, paying attention to a few core areas can make each visit more useful and more personal.

Why Doctors Value Pre-Visit Information
One of the things doctors notice most is that important details are often left out until the end of a doctor’s visit. A person may mention pain, dizziness, missed doses of medication, or a new symptom only as the appointment is ending. That can limit how much time there is to fully discuss the issue, review possible causes, or decide whether more evaluation is needed. In busy clinics, timing matters because even good medical information loses value when it arrives too late in the conversation.
Most primary care providers are not expecting a perfect summary. They do, however, benefit from a clear description of what changed, when symptoms started, how often they happen, what makes them better or worse, and whether anything new has happened with sleep, diet, stress, or medicine. That kind of detail supports more accurate care and may help determine whether the concern points toward a minor issue, a chronic condition, or something that needs testing or referral.
It also helps when patients plan. Writing down questions before appointments, bringing updated prescriptions, and noting any outside procedures, urgent care visits, or specialist recommendations can make the encounter more productive. For many doctors, the most important thing is not perfection. It is honest, organized communication that gives the care team a clearer picture of what is happening.
Minor Symptoms Can Be Important
Many people wait to talk about symptoms because they are not sure the issue is serious enough. They may expect it to pass, or they may feel worried about overreacting. But symptoms that seem small on their own can become more meaningful when they are viewed together with blood pressure, family history, age, medications, and recent test results. That is one reason primary care doctors encourage earlier conversations instead of delayed ones.
This does not mean every symptom signals a major disease. It means patterns matter. Fatigue, headaches, chest discomfort, changes in appetite, ongoing stomach concerns, or unexplained aches may be related to stress, routine illness, medical conditions, or something that requires closer follow-up. The purpose of treating patients in primary care is often to sort through that uncertainty carefully, not to jump to conclusions.
A thoughtful review may involve observation, lab work, repeat visits, imaging, or referral to specialists when needed. In that way, symptom reporting is not just about the current moment. It is part of how a provider builds context over time and protects long-term health decisions from guesswork.

Importance of Family Medical History
A detailed family medical history is one of the most overlooked parts of routine care. Yet the CDC notes that family health history can help a healthcare professional decide which screenings and other interventions may be appropriate, and when they should happen. This can be relevant for heart disease, high blood pressure, some forms of cancer, stroke, and other common diseases that show patterns across relatives.
For many patients, this information feels incomplete or hard to gather. They may know that a grandparent was sick but not know the diagnosis, the age of onset, or whether another family member had the same condition. Even partial information can still help. In family medicine and internal medicine, knowing whether a parent or sibling was diagnosed early with colon cancer, breast cancer, diabetes, or cardiovascular disease may shape screening conversations and preventive planning.
Doctors wish more people would update this information regularly rather than mention it once and never revisit it. Families change, new diagnoses happen, and that information may influence future preventive measures. In practical terms, a more complete record can support earlier monitoring, more personalized counseling, and a clearer understanding of where routine prevention may deserve extra attention.
Why Blood Pressure Deserves Attention
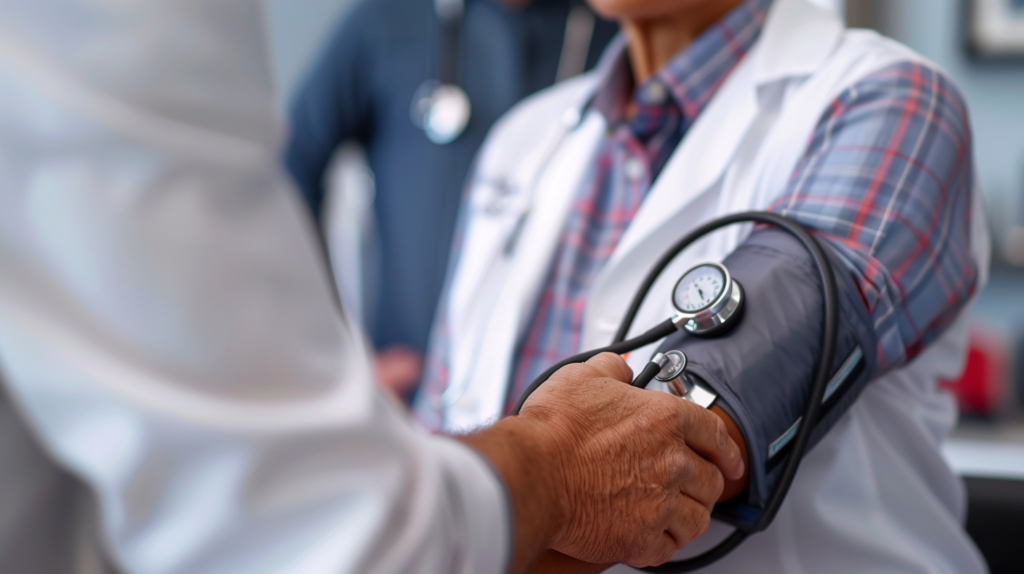
Among the many details covered in a routine checkup, blood pressure remains one of the easiest to dismiss. A reading may not feel urgent because high blood pressure often has no obvious symptoms. Yet NHLBI explains that a reading is considered high when it is consistently 130 systolic or 80 diastolic or higher, and many adults need regular checks through a healthcare professional.
That matters because patients sometimes focus only on how they feel, while hypertension can affect risk even when a person feels normal. In primary care, tracking numbers over time offers more value than reacting to one isolated reading. A clinician may compare in-office values, home readings, medication use, lifestyle factors, and cardiovascular risk before deciding whether observation, counseling, or specific treatment is appropriate.
What most doctors wish is simple: know your numbers, ask what they mean, and follow up when asked. Paying attention to blood pressure is not only about one diagnosis. It is part of broader prevention, especially when a person also has weight changes, stress, sleep concerns, diabetes risk, or a strong family history of vascular disease.
What Doctors Want Patients to Know About Prevention
Many people think preventive care is only about annual physicals. In reality, prevention includes screenings, counseling, risk review, vaccinations, and follow-up based on age, symptoms, history, and overall health goals. Public health guidance emphasizes that routine preventive care helps people stay well and detect some problems earlier, even when daily habits already seem healthy.
This is where a long-term relationship with primary care providers becomes valuable. A one-time visit can address an immediate concern, but continuity makes it easier to spot trends, compare old and new test results, and decide when a symptom is truly new versus part of a larger pattern. BluePoint Medical Group emphasizes prevention, early diagnosis, and ongoing care for exactly that reason.
Prevention also helps reduce the gap between what a patient experiences at home and what the clinic sees during a short appointment. Whether the topic is heart disease, cancer screening, metabolic risk, medication review, or sleep and stress, a preventive framework gives doctors and patients alike a better chance to make informed decisions before a concern becomes harder to manage.
How Honest Communication Supports Better Care
A surprising number of medical decisions depend on what patients choose to share. That includes alcohol use, supplements, missed doses, side effects, use of a new drug, internet-purchased treatments, and whether a person followed the last care plan. None of this is about judgment. It is about building the clearest possible record so the care team can make safer, better-informed decisions.
In practice, honesty can change how a diagnosis is considered or whether alternative treatments should even be discussed. Symptoms may look different when a patient mentions a recent medication change, a supplement interaction, or a home remedy that irritated. Likewise, a clinician may interpret abnormal test results differently if dehydration, poor sleep, recent illness, or skipped medication is part of the picture.
The internet gives many people fast access to health content, but not every website offers complete or reliable guidance. Bringing online questions into the exam room is often more useful than acting on them alone. Doctors generally prefer a direct conversation where concerns, expectations, and uncertainty can be reviewed together in context.

Personalizing Treatment in Primary Care
Patients sometimes assume that treatment begins only after a formal diagnosis. In reality, personalized care often starts earlier, during the process of narrowing possibilities and understanding goals. A primary care physician may review symptoms, risk factors, physical findings, medical information, and prior history before deciding whether monitoring, testing, medication, counseling, or referral is the right next step.
This matters because not every problem needs the same response. Some concerns are best managed through observation and routine follow-up. Others may call for lab work, imaging, prescriptions, or collaboration with specialists. BluePoint Medical Group’s model includes primary care, internal medicine, and diagnostic support, which can help patients move through evaluation in a more coordinated setting.
From a patient perspective, the important thing is to understand that personalized care is not about promising one ideal answer for every person. It is about matching the next step to the person in front of the clinician. Results vary, and treatment decisions depend on symptoms, risks, history, examination findings, and the need for follow-up.
Continuity Strengthens Care
One of the biggest differences between episodic care and true primary care is continuity. When a patient sees the same clinic over time, the record becomes more than a list of isolated complaints. It becomes a story of trends, responses, preferences, and risk factors. That context can improve follow-up after abnormal labs, medication adjustments, referrals, and recurring symptoms.
This kind of relationship also supports better conversations. A patient may feel more comfortable bringing up stress, weight changes, family concerns, or questions they avoided in the past. The care team may better recognize what is new, what is chronic, and what deserves more urgent attention. In many cases, that continuity is what turns scattered visits into more confident, informed care decisions.
For many patients, the value of this approach becomes clearer with time. Preventive planning, risk review, and chronic condition monitoring rarely happen in one perfect appointment. They tend to work better when there is an ongoing connection between the patient, the nurse, the physician, and the broader clinic team.
Timing of Testing and Follow-Up
Patients often want to know when a concern will lead to testing instead of watchful waiting. The answer depends on symptoms, history, physical exam findings, and how a concern is changing over time. In some cases, a clinician may recommend a diagnostic evaluation quickly. In others, repeating a measurement, tracking symptoms, or adjusting medication first may be more appropriate.
BluePoint’s patient education explains that diagnostic labs and related testing are used differently from general prevention. Preventive services look for risk or early disease based on age and guidelines, while diagnostic testing is used to evaluate a current concern or symptom. That distinction helps patients understand why one visit may focus on screening and another on determining the cause of a specific problem.
A referral does not necessarily mean something is seriously wrong. Sometimes it simply means that another perspective, a procedure, or a more specialized evaluation would improve the next step. Paying attention to follow-up instructions, portal messages, lab timing, and return visits is one of the practical habits that support safer care.

Key Takeaways After a Doctor Visit
The end of the visit is not the end of the care plan. It is the moment when instructions begin to matter most. Doctors often wish more patients would review the summary, confirm medication changes, schedule follow-up appointments, and ask what to do if symptoms change before the next visit. These steps may seem administrative, but they often shape outcomes just as much as the conversation itself.
It also helps to know what questions remain open. A visit may produce a working diagnosis rather than a final answer. It may also produce a plan to watch, repeat tests, or see how symptoms respond to treatment. In that setting, careful follow-through is part of informed care, not a sign that something went wrong.
For patients trying to protect long-term wellness, the most important thing is consistency. Small actions taken seriously over time often matter more than dramatic changes made once and forgotten.
FAQ
What do doctors wish patients paid more attention to before a routine visit?
Doctors usually want patients to track symptoms, bring updated medication information, and note any major health changes since the last visit. That preparation helps make the appointment more focused and supports more accurate decision-making.
Why is family medical history so important in primary care?
Family history can help a provider decide which screenings, counseling, or follow-up steps may be appropriate based on inherited and shared risk patterns. Even partial information about heart disease, cancer, or high blood pressure in close relatives can be useful.
Do I need to worry about blood pressure if I feel fine?
Possibly, because high blood pressure often has no obvious symptoms. Regular checks and follow-up with a healthcare professional are important when readings are elevated or when you have other cardiovascular risk factors.
When should I bring internet research to my doctor’s office?
Bring it any time you are using online information to make health decisions or question a treatment plan. A clinician can help place that information in context and explain whether it applies to your symptoms, history, and current care needs.
Conclusion
Long-term health rarely depends on willpower alone. It tends to work better when people have medical guidance, routine screening, and a place to revisit what is and is not working. In a setting built around preventive care, symptom review, and diagnostics, patients have more support for connecting daily choices with clinical follow-up. BluePoint Medical Group positions primary care as part of that long-range approach to prevention, evaluation, and wellness.
That support can make change feel more realistic. A clinician can review blood pressure, medications, sleep concerns, weight changes, family risk, and other markers that influence overall health, then help the patient decide what deserves attention now and what should be monitored over time. Not every concern requires the same response, and individual results vary, which is why decisions should be made with a licensed medical professional who can evaluate personal history and current needs.
Patients who pay closer attention to symptoms, prevention, family history, and follow-up often arrive at appointments with more clarity and leave with more direction. Contact BluePoint Medical Group to schedule a consultation and review your preventive care plan, current concerns, and next steps for more informed, personalized care.