Persistent pain can be frustrating because the symptoms are often real and disruptive long before the source is clear. A person may notice numbness, burning, weakness, radiating discomfort, or a persistent tingling sensation in the hands, arms, legs, or feet, yet still not know whether the problem involves the muscles, the nerves, the spine, or another part of the nervous system. When symptoms continue or start affecting daily activity, physicians often need more than a physical exam alone to understand what is happening.
That is where electrodiagnostic testing becomes valuable. Tests such as electromyography EMG and a nerve conduction study are commonly used to evaluate how nerves and muscles are functioning and whether the pattern of symptoms is more consistent with nerve damage, a muscle problem, or compression affecting the peripheral nervous system. BluePoint Medical Group describes nerve testing as a way to evaluate how well electrical signals move along a nerve pathway and to clarify whether symptoms match peripheral neuropathy, nerve compression, or another category of nerve disorders.
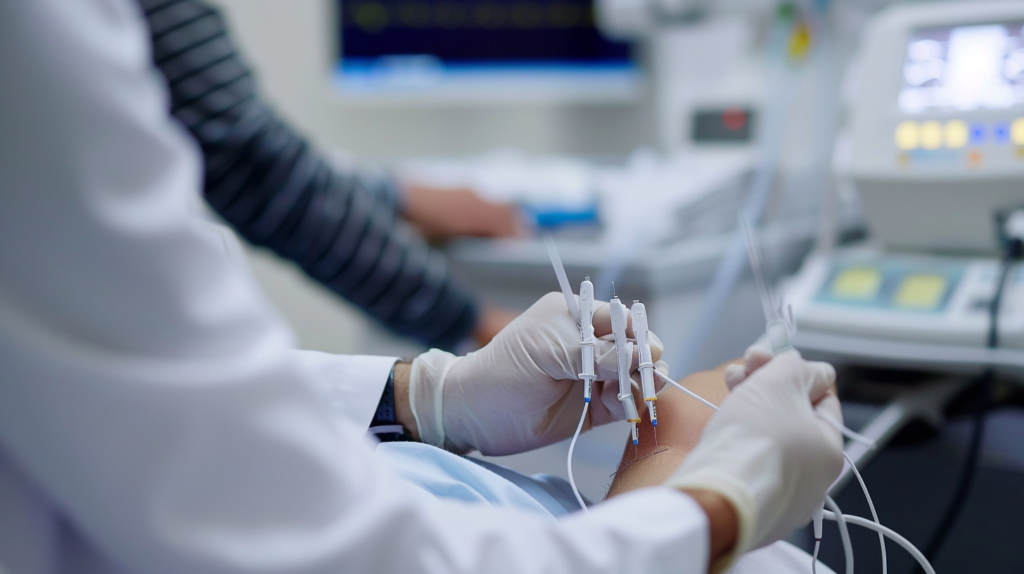
Why Persistent Pain May Indicate a Nerve Issue
Not all ongoing pain starts in the same place. Some symptoms come from inflamed joints or soft tissue, while others relate to peripheral nerves, irritated nerve roots, or a compressed spinal nerve. Pain that travels, feels electric, or is paired with numbness, tingling, or muscle weakness may raise concern that the problem involves the nerve itself rather than only the surrounding tissue. Cleveland Clinic notes that nerve conduction testing is often used when symptoms suggest peripheral nerve compression syndromes or neuropathy.
This distinction matters because the underlying cause changes the treatment approach. A patient with carpal tunnel syndrome, for example, may have compression of the median nerve, while another person with leg symptoms may have a pinched nerve near the spine or broader peripheral neuropathy related to diabetes, autoimmune disease, or another medical issue. When the source is uncertain, physicians may use nerve testing to narrow the possibilities before making a treatment plan.
What EMG and Nerve Conduction Studies Measure
EMG and nerve conduction testing are related but not identical studies. A nerve conduction study looks at how fast and how strongly a nerve sends electrical signals, often referred to as nerve conduction velocity and response strength. Johns Hopkins explains that nerve conduction testing measures the amount and speed of conduction of an electrical impulse through a nerve and can help determine nerve damage or destruction.
Electromyography, or EMG, evaluates the electrical activity of muscles at rest and during movement. It helps physicians see whether the problem appears to come from the muscle itself, the nerve supplying the muscle, or the connection between the two. In most cases, both tests are performed together because they provide complementary information about muscles and nerves and give a more complete view of muscle function and nerve health.
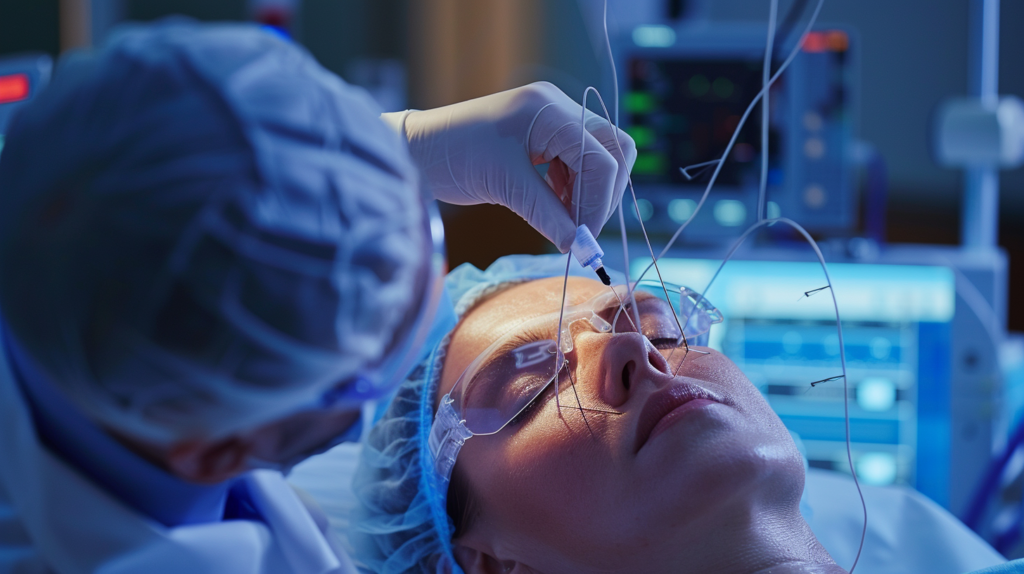
How Nerve Conduction Studies Detect Nerve Damage
During nerve conduction testing, surface electrodes are placed on the skin, and a brief electrical current is used to stimulate the nerve. The study measures how quickly and effectively the signal travels along the nerve, which helps physicians assess nerve conduction, conduction velocity, and whether the response suggests slowed or blocked transmission. If the nerve does not send signals at a normal speed, that may point toward nerve injury, compression, or disease affecting the nerve fibers.
This is especially useful when symptoms suggest focal entrapment or more widespread nerve dysfunction. Nerve conduction studies help physicians evaluate conditions such as carpal tunnel syndrome, peripheral neuropathy, and other problems affecting sensory nerves or motor fibers. Because the test can estimate severity and location, it often gives more practical information than symptoms alone.
What an EMG Reveals About Muscles and Nerves
An EMG test usually involves inserting a small needle called a needle electrode into selected muscles. The purpose is to assess whether there is abnormal electrical activity when the muscle is resting and when it contracts. This can reveal whether symptoms are more consistent with a nerve problem, a primary muscle disease, or another type of neuromuscular disorder. MedlinePlus notes that an EMG may cause mild pain, and some muscle soreness may occur for a few days after testing.
This information can be especially helpful when a patient has muscle weakness, cramping, or unexplained loss of function. EMG may support evaluation for muscle disorders, muscular dystrophy, myasthenia gravis, or motor neuron diseases such as amyotrophic lateral sclerosis, depending on the symptom pattern and exam findings. These tests do not stand alone, but they often help clinicians distinguish between disorders of the nerve, the muscle, and the nerve-to-muscle connection.
Conditions Nerve Testing Helps Evaluate
Nerve testing is commonly used when physicians are trying to understand ongoing pain, weakness, sensory changes, or suspected compression syndromes. Common examples include carpal tunnel syndrome, pinched nerves, peripheral neuropathy, and nerve injuries involving the arms or legs. It may also support evaluation for less common neuromuscular conditions, including Guillain-Barré syndrome, Charcot-Marie-Tooth disease, and selected autoimmune disorders that affect nerve signaling.
In some cases, these tests also help identify whether symptoms are coming from the spinal cord, spinal nerve roots, or the more distant peripheral nerves. That distinction matters because a person with back-related leg symptoms may need a different workup than someone with a diffuse stocking-glove pattern of numbness. Used carefully, the tests help move the conversation from vague pain to a more focused diagnostic pathway.
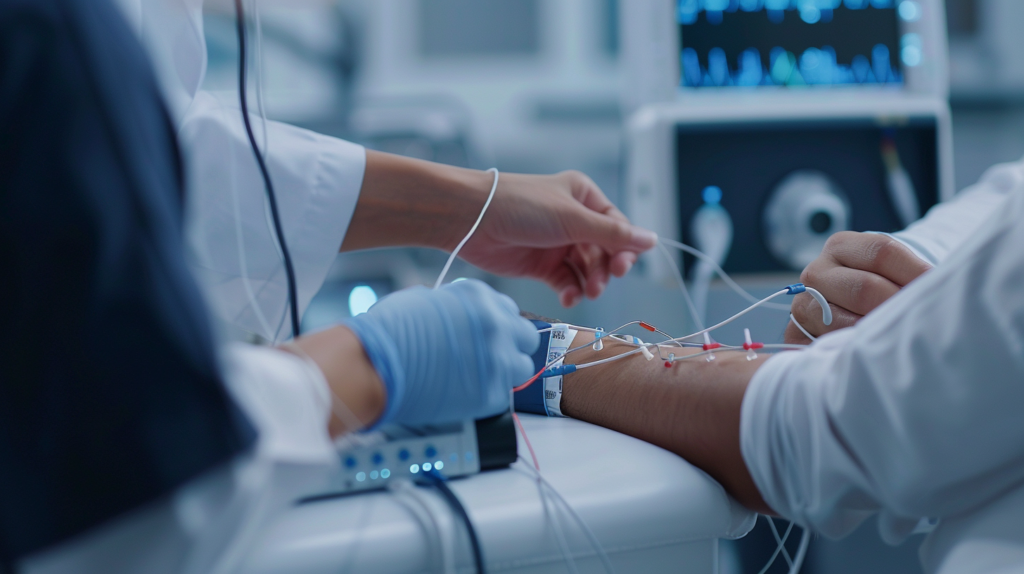
Can Nerve Testing Explain Numbness and Chronic Pain?
Often, yes. A patient with chronic pain, burning discomfort, or persistent tingling may have symptoms that overlap across many conditions, which is why a test-based evaluation can be useful. When physicians can see whether a nerve is conducting signals normally and whether the muscles are responding as expected, they are better positioned to determine whether there is a meaningful nerve-related explanation for the symptoms. Johns Hopkins notes that EMG and nerve conduction studies help detect the presence, location, and extent of diseases that damage nerves and muscles.
At the same time, these tests do have limits. They may not explain every pain syndrome, and some patients still need other tests, such as labs or imaging tests, depending on what the exam and history suggest. Good diagnosis is usually stepwise, combining test findings with symptoms rather than relying on one result alone.
What to Expect During Nerve Testing
For many patients, the biggest concern is what the testing feels like. During a nerve conduction study, you may feel a brief shock-like sensation from the electrical stimulation, often described as similar to static electricity. During EMG, the insertion of the needle may cause temporary discomfort, and the tested muscles may feel sore afterward for a short time. MedlinePlus describes the nerve conduction sensation as tingly and notes that soreness and bruising can happen after EMG.
Preparation is also important. Patients should tell their healthcare provider if they take blood thinners, have a pacemaker, or have conditions that could affect the procedure. That helps the team decide how to perform the test safely and interpret the findings more accurately.
FAQ
Does a nerve conduction study hurt?
You may feel a quick, mild shock-like sensation during the test because it uses brief electrical stimulation. Many patients tolerate it well, though the experience may still feel uncomfortable for a moment.
What is the difference between EMG and nerve conduction testing?
A nerve conduction study checks how well and how fast nerves send signals. EMG looks at the muscle’s electrical response and helps show whether the problem is coming from the nerve, the muscle, or both.
Can nerve testing diagnose carpal tunnel syndrome?
It may strongly support the diagnosis when symptoms and exam findings fit. These tests are commonly used to evaluate carpal tunnel syndrome and other nerve compression problems.
Will I need imaging tests too?
Possibly. Some patients need imaging tests or lab work in addition to EMG and nerve conduction studies, especially if the symptoms may relate to the spine, joints, or another medical condition.
Conclusion
The value of these studies is not just in naming a diagnosis. The real benefit is that test results may help identify the underlying cause of symptoms and guide a more precise next step. If the pattern suggests compression of the median nerve, for example, treatment may focus on splinting, ergonomics, medication review, or referral. If it points toward a generalized neuropathy or muscle condition, the plan may shift toward broader medical evaluation and long-term management.
At BluePoint Medical Group, this kind of testing fits into a broader diagnostic approach that emphasizes symptom clarification, informed decisions, and targeted follow-up. When pain, weakness, or sensory changes persist, accurate testing may reduce uncertainty and help patients move toward a more appropriate treatment plan instead of continuing without answers. Schedule a consultation with BluePoint Medical Group to discuss whether nerve testing is appropriate for your symptoms and what the results may mean for your next steps.